Oral Feeding until age 2 years
Bottle Feeding from 2 years to 3 1/2 years old
![]()
Oral Feeding until age 2 years
Bottle Feeding from 2 years to 3 1/2 years old
![]()
DJ was diagnosed with Tay-Sachs disease at the age of 18 months. We found out in reading about the course of Tay-Sachs that affected children gradually have trouble suckling and swallowing as they get older. One study said that their ability to swallow would dramatically decrease after age 3 years. We knew that feeding would become a major issue as the disease progressed.
DJ's neurologist had a specialist come and talk to us about long term feeding issues when he was diagnosed. At 18 months, DJ had a strong swallowing reflex and took all of his food by spoon and his liquids from a sipping cup. He had no history of reflux and had never had pneumonia. Aspiration was really not a problem. Except for his diagnosis, the doctor did not feel that DJ was a candidate for a feeding tube yet. We decided to commit to oral feedings for as long as we could.
![]() Oral Feeding until age 2 years:
Oral Feeding until age 2 years:
DJ was nursed until he was a year old. From the age of 5 1/2 months, he began taking solid foods. After he became "floppy" when he was 15 months old, we switched back to pureed foods. We found that almost anything can be put in a blender or small food processor. One of DJ's favorite meals included pancakes, maple syrup and chocolate milk. He also loved poached chicken ground up with cooked carrots, parsnip, and spinach.
We periodically check in with a nutritionist who monitors the caloric and nutritional value of DJ's food. She suggested providing adequate fluids and a normal, high-fiber diet to minimize his constipation. DJ takes in about 800 calories each day to maintain his weight. We give him Poly Vi Sol vitamin drops with iron, in his food a couple of times a week. Fortunately, DJ likes to eat and he takes a mixture of solid and pureed foods.
Drinking: It was important for DJ to get enough fluids to combat his problems with constipation. DJ started to drink Pediasure, a pediatric nutritional supplement, when he was 16 months old. DJ drank from a sipping cup until he was over 2 years old. We used thicker liquids like the Pediasure, nectars or yogurt drinks. We sometimes add a product called "Thick-it" or "ThickenUp" to juices, which we received from our nutritionist. Many parents add baby rice cereal or Hungry Jack potato flakes as thickeners.
Positioning: DJ took his meals in his high chair until he was 2 1/2 years old. We had to be careful to keep him relatively upright with his head in the midline position to prevent aspiration. DJ's high chair worked well because it could be tilted back at a slight angle. When we go to a restaurant, we sit him in his stroller or on our laps.
![]() Bottle Feeding from 2 years old to 3 1/2 years old:
Bottle Feeding from 2 years old to 3 1/2 years old:
As DJ's swallowing reflex weakened after his second birthday, it was increasingly frustrating to feed him. One meal by spoon would take up to 90 minutes per meal so we reverted back to the bottle. We learned a great feeding trick at the Home Care Session at the NTSAD Family Conference - try an infant feeder. We started feeding DJ with an Infa-Feeder by Sassy. The bottom of the bottle could be pushed upwards to bring the pureed food closer to DJ's mouth which made it easier for him to suck it up.
Gradually it became difficult to for DJ to take thin liquids like water or soup. We now added pureed food to thicken the liquid in his bottle. For example, we added 3 oz. of applesauce to every 4 oz. of Pediasure, or about 2 oz. mashed bananas to every 4 oz. of milk. We also tried another new method for feeding that came from a fellow parent. We took a regular baby bottle and cut the nipple to have a larger x-shaped opening.
By accepting these changes in DJ's feeding pattern, mealtimes became more enjoyable for me and less exhausting for DJ. One happy result was that he gained quite a bit of weight. By the time DJ was three years old, he weighed around 30 lbs.
Positioning: Good positioning is very important for oral feeding. DJ ate best when we supported his head and sat at a 45 degree angle or greater. He also ate well when placed in his KidKart wheelchair.
![]()
This section was extremely difficult for me to talk about. We knew that children with progressive neurological diseases like Tay-Sachs disease develop problems with feeding. As their muscles become weaker, they have more and more difficulty swallowing properly. As a result, they start to cough and gag during mealtimes. They can aspirate food into their lungs, leading to an increased risk of pneumonia.
Some signs that swallowing is becoming a real problem for an affected child include: difficult and exhausting feeding sessions, lost weight, chronic reflux, and frequent respiratory problems. Infrequent diapers may also indicate a problem with dehydration from lack of adequate fluid intake.
When DJ was first diagnosed, our doctors told us that feeding by tube would become necessary as the disease progresses. They told us to consider placing a feeding tube while DJ was healthy. Davis and I thought carefully about our options for long-term feeding, and decided against placing the feeding tube at 18 months. We decided to make the commitment to continue feeding by mouth. We worked with a nutritionist to achieve the best diet for DJ, and met with a speech therapist to learn positioning tactics.
Over the next two years, we returned periodically to this discussion over whether or not to place a feeding tube. We asked many parents in the PPG (Parent Peer Group) about their experiences with different feeding tubes, as well as about the end of their child's life. We found that there is is no single right answer because so much depends on the course of your child's illness. Some of our most difficult and painful discussions revolved around these long-term feeding issues.
There are three basic options: a G-tube, a NG tube, and letting nature take it's course.
1. G-tubes
Some parents decide to have a surgical procedure called a Gastrostomy. A small opening, called a stoma, is made by surgical incision into the stomach. A tube is inserted into the stoma. A small button caps the tube close to the surface of the tummy. Liquids and medicines can be delivered directly into the stomach through this tube. Parents say that the button is easy to care for.
Some affected children also have fundoplication done at the same time. Children with Tay-Sachs often suffer from G.E.R. (gastro-esophegeal reflux), where acid from the stomach is regurgitated up into the throat. Fundoplication is a surgical procedure in which part of the stomach is wrapped around the end of the esophagus to prevent the contents of the stomach from coming up.
For more information on enteral nutrition . . . Exceptional Parent magazine printed a series of five articles about enteral nutrition or feeding through a tube in 2001. They explained the basic procedures for placing a tube, tips on care for the tube and stoma, and notes on therapeutic positioining. For more information, link to: http://www.eparent.com/healthcare/nutrition_0.htm
2. NG tubes
Other parents chose a non-surgical option for their children. They decide to insert a nasogastric tube (NG tube). The NG tube goes in one nostril and down to the stomach. Liquid feedings and medicines are delivered directly into the stomach through the tube. The NG tube is easy to remove and is usually replaced once a month. The NG tube can be used as a short-term solution, to help children when they are sick to get extra fluids to prevent dehydration or for taking medicine when nothing stays down by mouth. Although more rare, the NG tube can also be used as a long-term solution, and children have thrived for years with a NG tube.
3. Letting nature take it's course
There is a third alternative for some parents. They feel very strongly against any medical intervention that would prolong their child's life when the quality of life has deteriorated. When their affected children were unable to swallow, could not tolerate their food, and essentially became non-responsive, they decided to let nature take its course. They chose not to actively prolong life. They let their child go without food and used drugs like morphine to ease pain and discomfort.
![]()
We knew that aspiration would be a major problem after DJ became 3 years old. His ability to swallow and suck has weakened considerably since August, 2000. We started using the suction machine to help him with thick mucous buildup during the night. His daily caloric intake also dropped over the past couple of months from over 800 calories to about 550 calories on average. On a slow day, DJ would get tired and it would take an hour for a full bottle. We have also been thickening his food for a while, but have reached a point where his bottles are half food and half liquid.
To prevent the aspiration from recurring, we decided to keep the NG tube in place. We found that we vould not return exclusively to oral feedings.
After a few months passed, the question of removing the NG tube and replacing it with a G-tube came up several times. We decided against gastrostomy surgery. Although we know that DJ is a surgical candidate despite his advanced age with the disease, he continues to have a strong protective cough reflex and no serious problems with reflux. We also found that DJ is not bothered by the NG tube and does not feel uncomfortable.
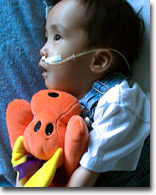
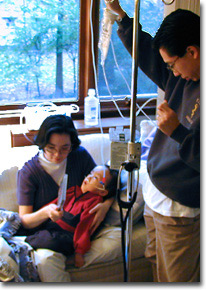
At the end of October, 2000, DJ was hospitalized for the first time with a serious illness. He had aspiration pneumonia at 3 1/2 years old. We left the hospital with a major change in our routine . . . DJ had a NG tube. He received liquid nutrition, antibiotics, and Diamox through the tube.
In this picture, DJ's NG tube is hooked up to an Enteralite feed pump. Davis is putting the bag filled with a can of Pediasure onto an IV stand. The feed pump will slowly deliver 8 ounces of Pediasure over about 40 minutes. We flush the NG tube with water afterwards. We keep a stethoscope around to make sure the NG tube is threaded into his stomach. We change the tape (tegaderm) holding the tube in place on his cheek weekly. The tube itself is replaced at the beginning of each month. (By the way, Akari is picking out a CD to play for DJ.) DJ's portable suction machine is located behind Akari's head. We keep a bottle of water around to flush out the tubing after we use it. We empty out the collection container each night and clean it with warm soapy water. We disinfect the collection container and tubing more thoroughly with a mixture of hot water and white vinegar once a week.
We are thankful that we are able to take care of DJ at home.